Fewer Delays, Faster Payments.
Revenue Cycle Management That Reduces Billing Delays and Gets You Paid Faster
Claim delays, payment gaps, and billing backlogs can put pressure on the whole practice. Vozo helps your team manage revenue workflows with better visibility, fewer missed steps, and steadier collections.






Why Choose Vozo for Revenue Cycle Management
Vozo supports revenue cycle teams with more organized workflows for claims, payments, and reimbursement follow-up.

Built for Daily Billing Flow
Vozo supports the real work behind revenue cycle operations, from claim submission to payment posting and patient balances, so teams can move work forward without relying on disconnected tools.

Helps Reduce Billing Delays
When claims, statements, and payments live in one connected workflow, staff can catch missing details sooner and keep revenue tasks from piling up.

Improves Follow-up Visibility
Vozo gives billing teams a clearer view of what was submitted, what is pending, what was paid, and what still needs action.
Revenue Cycle Features Built for Daily Billing Work
Clearing House
Claim submission should not turn into a manual, disconnected process. Vozo helps your team move claims through a connected clearing house workflow with less back-and-forth. Staff can track submission activity more clearly and act faster when something needs attention.
- Submit claims through a connected billing workflow
- Reduce repeated entry and manual file handling
- Track claim movement after submission
- Catch rejected items earlier for quicker correction
- Keep billing activity more organized across the team
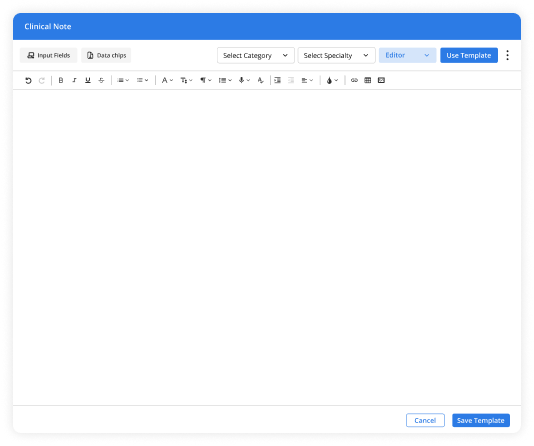
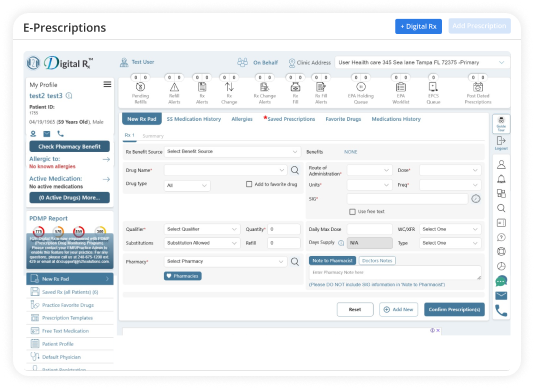
Insurance Claims
Insurance claims need speed, accuracy, and timely follow-up. Vozo helps practices manage claim activity in one place, from submission through status review. Teams get a clearer path to reimbursement with fewer missed actions along the way.
- Manage claims in one connected workflow
- Catch missing or incomplete items before submission
- Track status updates without extra spreadsheets
- Support faster follow-up on delayed claims
- Reduce rework tied to disconnected claim processes
Patient Payments
Patient collections become harder when payment activity is scattered. Vozo gives staff a simpler way to record, review, and manage patient payment workflows. Balances stay easier to track, and collection work stays more consistent across the day.
- Record patient payments in one place
- Keep balance updates visible for staff review
- Reduce missed follow-up on open patient amounts
- Support smoother front-desk and billing coordination
- Help practices stay more current on collections


Patient Statements
Statements should go out on time and reflect balances clearly. Vozo helps practices manage patient statements in a more structured billing workflow. This gives staff better control over statement timing and reduces confusion around what patients owe.
- Generate statements tied to patient balances
- Support more timely billing communication
- Reduce missed statement cycles and delays
- Help patients understand what they owe
- Keep statement activity easier to review
Accounts Receivable
Revenue teams need a dependable view of charges, payments, and outstanding balances. Vozo helps staff track accounts clearly so follow-up and collections stay on track.
- View outstanding balances and payment history in one place
- Track aging accounts and prioritize follow-up
- Support cleaner collection workflows across the team
- Reduce missed follow-up on unpaid claims and balances
- Help staff stay on top of revenue recovery

Features
More Features
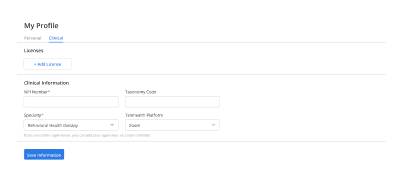
Claim Status Tracking
Track claim progress, delays, and next steps in one place so staff can follow up faster and miss less.
Denial Management
Identify denied claims sooner, organize follow-up clearly, and reduce revenue loss caused by missed corrections and resubmissions.
Payment Posting
Post payments faster with clearer visibility into remittance details, patient balances, and outstanding billing activity across accounts.
Eligibility Verification
Confirm coverage before visits to reduce claim issues, front-desk confusion, and payment delays caused by incomplete insurance details.

Coding Support
Improve coding accuracy before submission to reduce preventable claim errors and billing rework.

Account Follow-Up
Track unpaid claims, open balances, and pending next steps more clearly so revenue does not stall across aging accounts.
How it works
Create Your Vozo EHR Account in 3 Simple Steps
Set up your practice fast, keep your workflow familiar, and start charting confidently.
1
Create account
Get started with a setup process that feels clear and manageable.
2
Set up billing workflow
Add your revenue settings, payment processes, and team responsibilities with less friction.
3
Start managing revenue
Submit claims, track payments, and stay on top of billing work with better visibility.
Testimonials
Success Stories From Our Users
See Why Behavioral Health Providers Love VOZO
— Dr. Emily Ross, Clinical Psychologist
“Finally, an EHR that understands therapists. From notes to sessions, everything feels intuitive and built for real clinical workflows.”
— Sofia Mendes, LCSW
FAQ
What providers ask about revenue cycle management
Vozo helps reduce claim delays by connecting clearing house activity, insurance claims, payment posting, and follow-up in one workflow.
Vozo supports patient payments, card transactions, statements, and ledger activity in one place. This makes it easier for staff to collect balances, review account history, and keep patient billing communication more consistent.
ERA and EOB workflows help billing teams review payer responses, post payments, identify variances, and follow up on denied or underpaid claims. This improves payment visibility and reduces manual billing work.
Vozo includes fee schedule and patient ledger tools that help practices maintain charge consistency, review account activity, and reduce confusion across front-desk and billing workflows.
Vozo can support practices with dedicated billing specialists, billing managers, and billing and coding services. This helps reduce internal workload, improve claim quality, and keep revenue tasks moving more consistently.
Vozo helps practices reduce delays, improve billing visibility, and keep revenue work moving with less manual effort.
✓ No Credit Card Required